American Cancer Society
Experts explore emerging evidence linking diabetes and cancer
ATLANTA—June 16, 2010—A new consensus statement of experts assembled by the American Diabetes Association and the American Cancer Society reviews emerging evidence that suggests cancer incidence is associated with diabetes as well as certain diabetes risk factors and treatments. The new report reviews the state of science concerning the association between diabetes and cancer incidence/prognosis; risk factors common to both diseases; possible biologic links between diabetes and cancer risk; and whether diabetes treatments influence the risk of cancer or cancer prognosis. In addition, the report outlines key unanswered questions for future research.
Diabetes and cancer are common diseases that have a tremendous impact on health worldwide. Epidemiologic evidence suggests that people with diabetes are at a significantly higher risk of many forms of cancer. Type 2 diabetes and cancer share many risk factors, but potential biologic links between the two diseases are not completely understood. Moreover, evidence from observational studies suggests that some medications used to treat hyperglycemia are associated with either an increased or reduced risk of cancer. Against this backdrop, the American Diabetes Association and the American Cancer Society convened a consensus development conference in December 2009. After a series of scientific presentations by experts in the field, the writing group independently developed a consensus report to address important questions: Is there a meaningful association between diabetes and cancer incidence or prognosis? What risk factors are common to both cancer and diabetes? What are the possible biologic links between diabetes and cancer risk? And do diabetes treatments influence cancer risk or cancer prognosis?
For each of these areas, the authors were asked to address current gaps in evidence and potential research and epidemiologic strategies for developing more definitive evidence in the future. Below is a summary of their findings and recommendations.
Diabetes (primarily type 2) is associated with an increased risk of some cancers (liver, pancreas, endometrium, colon/rectum, breast, and bladder). Diabetes is associated with a reduced risk of prostate cancer. For some other cancer sites, there appears to be no association or the evidence is inconclusive.
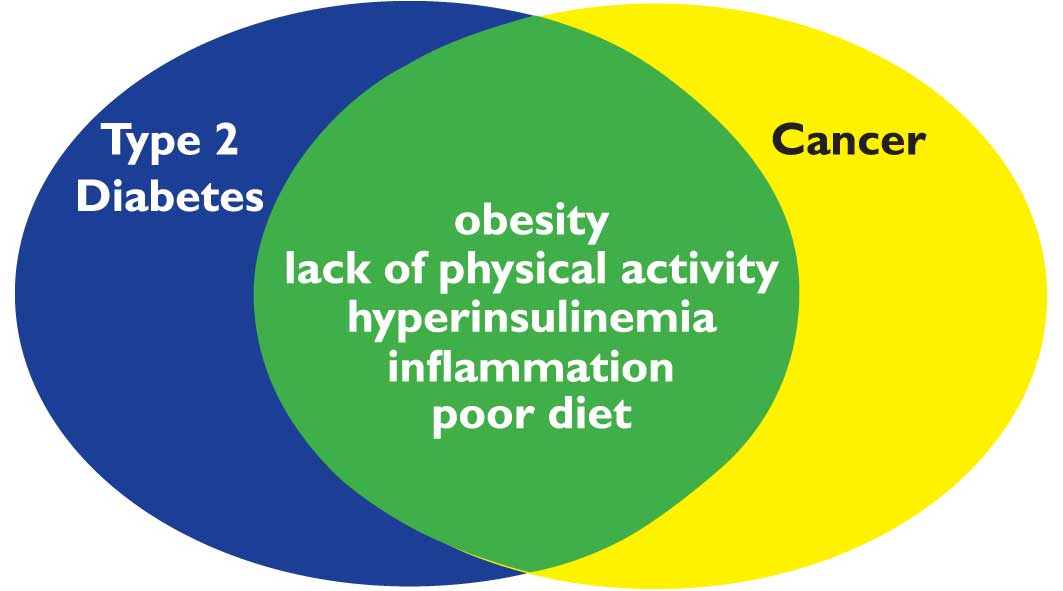
The association between diabetes and some cancers may be due in part to shared risk factors between the two diseases such as aging, obesity, diet, and physical inactivity.
Possible mechanisms for a direct link between diabetes and cancer include hyperinsulinemia, hyperglycemia, and inflammation.
A healthy diet, physical activity, and weight management reduce the risk and improve outcomes of type 2 diabetes and some forms of cancer and should be promoted for all.
Patients with diabetes should be strongly encouraged by their health care professionals to undergo appropriate cancer screenings as recommended for all people of their age and sex.
The evidence for specific drugs affecting cancer risk is limited, and observed associations may have been confounded by indications for specific drugs, effects on other cancer risk factors such as body weight and hyperinsulinemia, and the complex progressive nature of hyperglycemia and pharmacotherapy in type 2 diabetes.
Although still limited, early evidence suggests that metformin is associated with a lower risk of cancer and that exogenous insulin is associated with increased cancer risk. Further research is needed to clarify these issues and evaluate the possible association of insulin and other diabetes medications with the risk of cancer.
Cancer risk should not be a major factor when choosing between available diabetes therapies for the average patient. For selected patients with a very high risk of cancer occurrence (or for recurrence of specific cancer types), these issues may require more careful consideration.
Many research questions remain.
“Traditionally there hasn’t been much overlap between research in cancer and in diabetes,” says Edward Giovannucci, MD, SCD, co-chair of the consensus report group. “But recently it’s become clearer that there are fascinating links between the two. Our summary may raise more questions than provide answers, but we hope that it will spur additional studies.”
“The vast majority of patients with diabetes need not consider cancer risk when weighing their diabetes therapy options,” added David M. Harlan, MD, co-chair of the consensus report group, “Only patients with a very high risk for cancer occurrence, or re-occurrence, may wish to carefully consider their options. Even then, the association appears to exist for some cancer types, and not for others. We have much to learn.”
 Parsi Teb Physical and Mental Health Journal
Parsi Teb Physical and Mental Health Journal